Kenya and Satoru Meet Again but Meet a Child That Breastfeeding From Satoru Fanfic
- Inquiry article
- Open Admission
- Published:
Patterns and determinants of breastfeeding and complementary feeding practices in urban informal settlements, Nairobi Republic of kenya
BMC Public Health volume 11, Article number:396 (2011) Cite this commodity
Abstract
Background
The World Health Organisation (WHO) recommends exclusive breastfeeding during the first six months of life for optimal growth, development and health. Breastfeeding should continue up to two years or more than and nutritionally acceptable, safe, and appropriately-fed complementary foods should exist introduced at the historic period of six months to see the evolving needs of the growing infant. Little evidence exists on breastfeeding and baby feeding practices in urban slums in sub-Saharan Africa. Our aim was to appraise breastfeeding and babe feeding practices in Nairobi slums with reference to WHO recommendations.
Methods
Data from a longitudinal study conducted in two Nairobi slums are used. The study used information on the start twelvemonth of life of 4299 children built-in between September 2006 and January 2010. All women who gave nativity during this period were interviewed on breastfeeding and complementary feeding practices at recruitment and this information was updated twice, at four-monthly intervals. Cox proportional risk analysis was used to determine factors associated with cessation of breastfeeding in infancy and early introduction of complementary foods.
Results
There was universal breastfeeding with almost all children (99%) having ever been breastfed. However, more a third (37%) were not breastfed in the beginning hour following delivery, and forty% were given something to drinkable other than the mothers' chest milk inside three days subsequently delivery. About 85% of infants were yet breastfeeding by the stop of the xith month. Sectional breastfeeding for the outset half dozen months was rare as only about 2% of infants were exclusively breastfed for six months. Factors associated with sub-optimal babe breastfeeding and feeding practices in these settings include child's sex; perceived size at birth; mother'south marital status, ethnicity; education level; family planning (pregnancy desirability); health seeking behaviour (place of delivery) and; neighbourhood (slum of residence).
Conclusions
The study indicates poor adherence to WHO recommendations for breastfeeding and infant feeding practices. Interventions and farther research should pay attention to factors such every bit cultural practices, access to and utilization of health care facilities, kid feeding education, and family planning.
Background
The starting time two years of life are critical stages for a child's growth and evolution. Any damage caused by nutritional deficiencies during this flow could lead to impaired cognitive development, compromised educational achievement and depression economic productivity [1–3]. Poor breastfeeding and complementary feeding practices, together with high rates of morbidity from infectious diseases are the prime proximate causes of malnutrition in the commencement 2 years of life. Breastfeeding confers both brusque-term and long-term benefits to the child. It reduces infections and mortality among infants, improves mental and motor development, and protects against obesity and metabolic diseases later on in the life course [3–7].
The WHO recommends exclusive breastfeeding in the first 6 months, beginning from the get-go hour of life, to run into the infant'due south nutritional requirements and accomplish optimal growth, development and health. The mother is advised to keep breastfeeding upward to two years of age or more and brainstorm nutritionally acceptable, safety, and appropriately-fed complementary foods at the historic period of six months in order to see the evolving needs of the growing infant [6]. The WHO/UNICEF global strategy on infant and young child feeding practices aims to promote optimal breastfeeding and complementary feeding practices, through various initiatives for example the Babe Friendly Hospital Initiative (BFHI) and the International Breastfeeding Code [eight]. Interventions promoting optimal breastfeeding could prevent 13%, while those promoting optimal complementary feeding could preclude another 6% of deaths in countries with high bloodshed rates [5].
Poor breastfeeding and complementary feeding practices have been widely documented in the developing countries. Only nigh 39% of infants in the developing countries, 25% in Africa are exclusively breastfed for the outset 6 months. Additionally, 6% of infants in developing countries are never breastfed [9]. In Kenya, according to Kenya Demographic and Health Survey 2008-2009 [ten], 32% of children under the age of six months are exclusively breastfed, improving from only 13% in 2003 [11]. As a result, substantial levels of child malnutrition and poor child wellness and survival have been documented in Republic of kenya [xi]. Deriving from the wide principles of the joint WHO and UNICEF's Global Strategy for infant and young child feeding developed in 2002 [8], the government of Kenya is implementing a strategy aimed at improving infant and young kid feeding practices in Kenya. The strategy is actualized through revitalization of the BFHI [12].
Urban poor settlements or slums nowadays unique challenges with regards to child health and survival. Slums in sub-Saharan Africa are expanding at a fast rate, and the majority of urban residents now live in slum settlements, [xiii]. These slums are characterized past poor environmental sanitation and livelihood conditions [14–16]. Contrary to the long-held conventionalities that urban residents are advantaged with regards to wellness outcomes, urban slum dwellers tend to take very poor wellness indicators [14, 17, 18]. For example, in Republic of kenya, slum children are reported to be sicker and to take higher bloodshed rates than any other sub-grouping in Kenya including the rural areas [xiv]. In line with this, infants built-in to mothers that reside in the urban slums may be exposed to sub-optimal breastfeeding and complementary feeding practices.
Various factors associated with sub-optimal breastfeeding and complementary feeding practices have been identified in various settings. These include maternal characteristics such as age, marital status, occupation, and education level; antenatal and maternity health care; health education and media exposure; socio-economical status and surface area of residence; and the kid's characteristics including birth weight, method of delivery, birth club, and the use of pacifiers [19–21]. However, in that location are conflicting findings with regards to the consistency of the associations and the magnitude of the effects [20, 22–25], suggesting that the context may be of import when trying to isolate characteristics and practices that may be amenable to interventions. At that place is limited evidence on breastfeeding and babe feeding practices in urban slums in sub-Saharan Africa since few studies have focused on urban slums. Although there is national level bear witness on breastfeeding and infant feeding practices, the data for urban areas is not disaggregated, and hence, the famine of evidence on practices in urban slums. In this study, nosotros accept nerveless longitudinal data and assessed infant feeding practices with reference to WHO recommendations, in two slums in Nairobi, Republic of kenya, and their determinants.
Methodology
Study setting and data source
The study was carried out in 2 urban slums of Nairobi Republic of kenya (Korogocho and Viwandani) where the African Population and Health Research Eye (APHRC) runs a health and demographic surveillance organization; the Nairobi Urban Wellness and Demographic Surveillance Organisation (NUHDSS). The two slum areas are densely populated (63,318 and 52,583 inhabitants per foursquare km, respectively), and are characterized by poor housing, lack of basic infrastructure, violence, insecurity, high unemployment rates, and poor health indicators [14, xv, 17]. The socio-economical status of the two slums differs slightly: Viwandani has relatively higher levels of education and employment as beingness located in the industrial surface area, information technology attracts migrant workers. On the other hand, the population of Korogocho is more stable since on average, residents in the area have lived the expanse for a longer menstruation than Viwandani residents. Approximately ii thirds of married men live with their spouses in Korogocho, compared with half in Viwandani.
The NUHDSS involves a systematic recording (every four months) of vital demographic events including births, deaths and migrations occurring among residents of all households in the NUHDSS surface area, since 2003. Other data that are collected regularly include household avails, morbidity, and highest educational attainment. This paper is based on data from a maternal and kid wellness component of a broader longitudinal report entitled "Urbanization, Poverty and Wellness Dynamics in sub-Saharan Africa" that was nested within the NUHDSS. The written report started in February 2007 and concluded in December 2010. All women who gave nascency since September 2006 and their children were enrolled in the study and were followed up every 4 months to obtain data including self-reported health status, breastfeeding, complementary feeding practices, vaccination and health intendance. Data on socio-economic status was extracted from the NUHDSS database and linked to the study participants through their household identifier.
Information collection & sample
The data presented in this paper were nerveless at baseline and during the first ii updates, four months autonomously, for each child recruited between February 2007 and May 2009. Therefore, the follow-up period for each child was on average nine months and the average historic period of the children at the second update was xv months. However, we restrict our analyses to the offset year of life for all 4,299 children who were enrolled in the written report. Tabular array i presents the sample size for the children involved in the study and the data collection dates. Six cohorts of children enrolled during the study period are included.
Variables
a. Dependent variables
The 2 dependent variables are abeyance of breastfeeding and introduction of complementary foods (liquids and solids). Cessation of breastfeeding is a fourth dimension-dependent variable indicating the age when breastfeeding was stopped. Introduction of complementary foods is also a fourth dimension-dependent variable indicating the historic period at which complementary foods (either liquids or solids other than breastmilk) were introduced. Children who entered the study subsequently the events (breastfeeding cessation or initiation of complementary foods) had occurred had their information updated retrospectively. Virtually ane% of children were never breastfed and were excluded from survival assay. Children who did not have their information updated due to loss to follow-up were excluded from the study.
b. Independent variables
The independent variables were: the child's sex; the mother's historic period (< 25 years, 25-34 years, 35+ years); the marital status of the female parent (in union i.e. currently married or living with someone; previously in wedlock; and never married/in union); the ethnicity of the mother (Kikuyu, Luhya, Luo, Kamba, and other tribes); the highest level of education (none, principal, secondary or college); and parity (one, 2, 3+); pregnancy desirability of the index child (wanted at the fourth dimension of conception, wanted later and never wanted,); the place of delivery (health facility, home or traditional nativity attendant [TBA]); the mother'due south perception of the child'due south size at nascency (normal, smaller than normal, larger than normal); the socio-economic status of the household; and the slum of residence (Viwandani or Korogocho). The household socioeconomic status was defined using the household monthly expenditure per capita, taking a kid to be the equivalent of half an adult. The expenditure data used was obtained from the poverty component of the Urbanization, Poverty and Wellness Dynamics report, and was collected in the same year as the data for the dependent variables above. This variable was recoded as tertiles of "poorest", "middle" and "least poor".
Data Analysis
The survival analysis of the elapsing of breastfeeding and the fourth dimension to introduction of complementary foods is presented using Kaplan-Meier survival curves. Cox regression assay was performed to decide factors associated with breastfeeding abeyance during infancy and early introduction of complementary foods. Some independent variables had missing values, mainly maternal level variables such as the mother'due south age, ethnicity, the highest level of education; and the household's socio-economic status. A missing category was created in the multivariate analysis to go on all cases in the analysis (though results for missing category are not shown). In all cases, except the household expenditure variable, the number of cases with missing information was less than 10%. About 1-tertiary of the participants were missing data on household expenditure, therefore imputation using a linear interpolation ciphering procedure was used. A p-value of less than 0.05 was used as the cut-off for statistical significance.
Ethical Considerations
The Urbanization, Poverty and Health Dynamics study was canonical by the Ethical Review Lath of the Kenya Medical Inquiry Institute (KEMRI). The field workers were trained in research ethics and obtained informed consent from all respondents. The NUHDSS has besides been approved past KEMRI's Ethical Review Board. Verbal consent is routinely obtained from all the NUHDSS respondents.
Results
Sample Characteristics
About all the children (99%) were always breastfed; however, more than a third (37%) were not breastfed in the offset hour following delivery. The chief reasons given for not initiating breastfeeding immediately were: little or no breastmilk (35%); baby being comatose/tired (23%); babe being sick (13%); and mother being sick (9%). Ii in five of the children were given something to drinkable other than the mothers' breast milk within 3 days following delivery. The main reasons given were that the mother had footling or no breast milk (42%) or that the kid had an upset stomach (32%). During each data collection round, mothers and other caregivers were asked if the kid was being given any liquid or solid food to complement breastfeeding, with the recollect period being the final three days. The most common complementary foods existence given to children before the historic period of half dozen months were: plain water (56%), with most children on information technology having been given within the first month (69%); porridge (54%), with near children on it having been introduced between the second and third months (64.seven%); fresh or powdered milk (45%) with most children on it also having been introduced between second and third months of life (57%); and sweetened/flavoured water (41%), with most of children on information technology having been introduced inside the first month of life (78%). The main reason given for introducing complementary foods to children below six months was that the mother had no or piddling breast milk (approx 40%). About two-thirds knew that complementary feeding should be started at 6 months while well-nigh xxx% indicated they should be started before 6 months.
Survival Assay
Abeyance of breastfeeding and introduction of complementary foods
Effigy 1 shows Kaplan-Meier survival curves for probability of continuing breastfeeding at specific ages. Well-nigh all of the infants were started on breastfeeding, and virtually 85% of the infants were all the same breastfeeding by the finish of the 11th month. Figure ii illustrates Kaplan-Meier survival curves for time to introduction of complementary foods. Nearly all (98%) of children had been introduced to complementary foods (either liquids or solids) by the age of 6 months. Liquids were introduced much earlier than solids; the mean age of introduction of liquids was 1 month while that for solids was 3 and a half months.
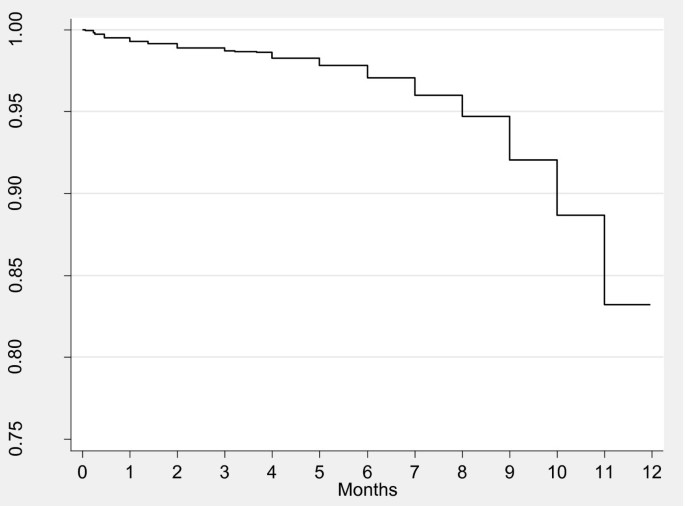
Probability of continuing breastfeeding for specific ages, Nairobi informal settlements, Kenya.
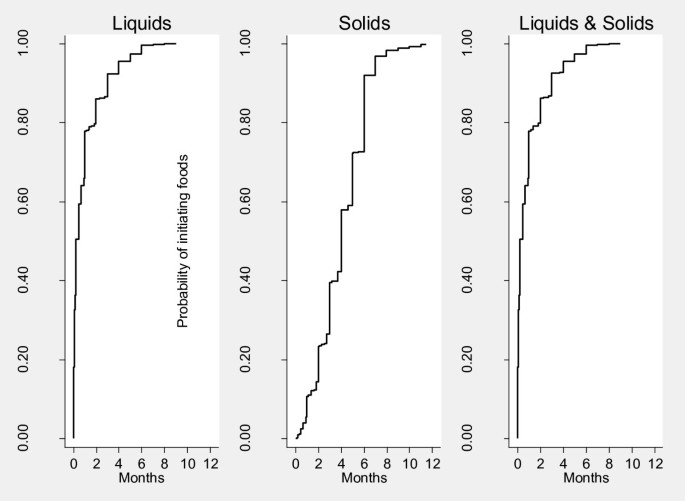
Probability of initiating complementary foods for specific ages, Nairobi informal settlements, Kenya.
Proportional Hazards Regression
In the multivariate analysis, the factors significantly associated with cessation of breastfeeding during infancy were the mother'southward marital status, her ethnicity, and her highest level of education and the perceived size of the kid at nascence (p < 0.05, respectively). The mother's age was marginally associated (p > 0.05 < 0.1) with the duration of breastfeeding. When other factors were controlled for, mothers who were previously in spousal relationship and those never in marriage had shut to 3 and two fold higher hazards of stopping breastfeeding earlier the age of 12 months respectively compared to mothers in union. Luhya, Luo and mothers of other ethnic groups were more likely to stop breastfeeding early (Hazard Ratios: 1.half dozen, 1.viii. and 2.1, respectively), compared to Kikuyu mothers; mothers with secondary or 3rd didactics level had 40% lower hazards of stopping breastfeeding compared to those with less than secondary level education; and children who were perceived as larger than normal were 40% less likely to cease breastfeeding before the age of 12 months (Tabular array ii).
Factors associated with early introduction of complementary foods (before the historic period of six months) at multivariate level include child's sexual activity; female parent'due south marital condition, ethnicity, and education level; pregnancy desirability; place of commitment; and slum of residence (p < 0.05, respectively). Boys were more than likely to be introduced to foods early on; mothers never in union had 23% higher hazards of introducing complementary foods before half dozen months of age; Luos, Luhyas and other ethnic groups were more than probable to innovate foods early on; mothers with at least secondary level education had 10% lower hazards of introducing foods early on; children who were non wanted at formulation but wanted later had vii% lower hazards of being introduced early; and mothers in Viwandani had ten% lower hazards of introducing complementary foods early on compared to mothers in Korogocho (Table 3).
Give-and-take
This study has documented breastfeeding and babe feeding practices in two slum settings in sub-Saharan Africa. It has also identified the factors associated with sub-optimal breastfeeding and baby feeding practices in these ii slum settings. The study finds that though there is almost universal breastfeeding, exclusive breastfeeding is rare. Complementary foods are initiated too early; only two percent of children were exclusively breastfed before the age of six months and the mean age of introduction of complementary foods was i month.
In our study, nosotros come across an overall picture of universal breastfeeding with the bulk of infants breastfed for at to the lowest degree 12 months. These findings are similar to findings in other developing countries [9, 26]. However, this moving picture masks the unwelcome finding that the WHO recommendations with regards to breastfeeding and introduction of complementary food were largely not adhered to. Early initiation of breastfeeding following delivery, equally recommended by the WHO is non universally existence proficient in developing countries, despite the importance of colostrum in providing the infant with rich nutrients. The findings that shut to 40% of the infants were not breastfed within one hour post-obit delivery are in agreement with findings from studies in other developing countries including Uganda, India and Bangladesh [xx, 26, 27]. In our setting, the main reasons stated for failure to introduce babies to breast milk immediately after birth were health-related including the mother having bereft milk. This has too been documented in other studies [22]. Other cultural factors have been noted in other settings such as Nigeria, for example the belief that colostrum is dirty milk, hence harmful to the baby, a belief that the mother should residue and clean up get-go, and performance of rituals and prayers earlier the infant starts breastfeeding [28]. In our study though, cultural factors did not characteristic in the responses from the women, supposedly considering our study was a quantitative, rather than qualitative written report.
In this written report complementary foods were initiated as well early, despite two thirds of the women in our report being enlightened of the WHO recommended time to initiate complementary feeding. This is in line with previous studies conducted in rural Kenya, Republic of malaŵi and Uganda [26, 29, thirty], and in some other slum settings in the developing world [31, 32]. In a study conducted in the late 1990s on the determinants of kid nutritional status in six African countries, Madise et al. reported very depression levels of exclusive breastfeeding among infants under the historic period of 4 months with percentages ranging from ii percent in Nigeria to nigh 34% in Tanzania [33]. The few studies that take looked at slum settings particularly in Asia paint a similar pic [31, 32]. The finding showing the persistence of early introduction of complementary feeding in the region is critical given the importance of sectional breastfeeding to child health. Exclusive breastfeeding protects confronting infections such as gastrointestinal and respiratory infections, and enhances motor evolution in the kid [four, 34, 35]. In a study using data from Botswana which examined the clan between breastfeeding, morbidity, and malnourishment, Chikusa (1991) found that children anile 4 months or younger who had been weaned had more than eleven times the odds of having diarrhea compared with those who were still being breastfed [36]. The main reason cited for introducing complementary food early was the mother's perception of bereft chest milk. This finding is in line with other studies from other settings which take shown that the perceived lack of sufficient breast milk is a main reason for early breastfeeding cessation or early on introduction of complementary foods [31, 37, 38].
The variables associated with the cessation of breastfeeding during the first year of the kid's life include the mother's marital status, her ethnicity, and her level of instruction, and perceived size at birth. The association betwixt marital condition and early abeyance of breastfeeding has been reported in many studies with conflicting results [22, 23]. In this study, women who were not in union, particularly those who were formerly married were more likely to stop breastfeeding their infants than women who were in union. It has been suggested that the clan betwixt marital status and breastfeeding cessation may be due to the presence or absence of social, emotional and economic support of a partner [39]; however, these factors were not assessed in our study. A more plausible reason in Kenya, where HIV is high, is that a disproportionately big number of formerly married women are HIV positive and many women in this state of affairs were until recently brash to exclusively breastfeed their baby for half-dozen months and so to rapidly wean [forty].
The evidence of the association between a female parent's level of education and the duration of breastfeeding also varies [twenty, 24, 25]. In this study, lower than secondary level didactics was associated with earlier cessation of breastfeeding. While information technology is not very clear why this is the case, higher educational activity may be associated with college cognition and practice of positive health behaviour. Higher HIV prevalence among those with less than secondary level didactics, especially those with no education at all in our setting [41] may exist associated with early cessation of breastfeeding. We also observed an clan betwixt ethnicity and breastfeeding cessation. All other ethnic groups apart from the Kamba were more probable to stop breastfeeding their infants compared to Kikuyu women. There is no established reason for this but information technology could be multi-factorial, including cultural practices related to breastfeeding and child rearing. Further, HIV prevalence, which may affect breastfeeding practices, has also been documented as college amid the Luo and Luhya ethnic groups in this slum setting compared to the Kikuyu ethnic grouping [41]. Additionally, prove from the study areas indicates that Kikuyus have lower fertility compared to other ethnic groups. Prolonged breastfeeding may explain or be explained by lower fertility. Mothers who get pregnant while breastfeeding are more probable to end but, as well mothers who breastfeed for longer period have lower chances of getting significant [42]. Additionally, better child health outcomes have also been documented among the Kikuyu's compared to other indigenous groups in this written report setting [xiv] and our findings may indicate that the Kikuyus have better wellness-related behaviours and practices than almost of the other indigenous groups in the study area. The association betwixt birth size and the duration of breastfeeding has not been studied in depth. Our report constitute that children who were perceived to be larger at nativity were less likely to exist stopped from breastfeeding earlier. This is similar to a United states study, infants who were breast-fed for less than 4 months were smaller at nativity than those who were breast-fed for iv months or more [43]. The factors behind this association in our study setting need farther investigation.
Predictors of early on introduction of complementary foods include the kid's sex; the mother's marital condition, her ethnicity, and her level of education; the desirability of the pregnancy of the index child, the identify of delivery and the slum setting. Boys were more likely to exist introduced to complementary feeding early compared with girls. Anecdotal evidence indicates that boys are introduced to complementary foods early on considering breast milk alone does not meet their feeding demands. Having never been in union/married was associated with higher risk of early introduction of complementary foods. A positive association between beingness married and exclusive breastfeeding has been documented in other studies [44]. As in the instance of the elapsing of breastfeeding, this may be associated with social, emotional and economic support of a partner [39]. Similar to the finding related to the duration of breastfeeding, all other ethnic groups apart from the Kamba group, were more probable to initiate complementary foods earlier than the Kikuyus. This may be related to cultural practices and other factors such as HIV condition equally described for duration of breastfeeding. While a few studies have linked the mother's education with early introduction of complementary foods [27], similar to our report, the negative influence of a female parent's low education on early on introduction of complementary foods has been observed in many studies in other settings, suggesting a need for education and health promotion to modify these harmful feeding practices [21, 45, 46].
Slum of residence, was associated with the timing of introduction of complementary foods. Mothers from Viwandani, were at lower risk of introducing complementary foods before six months. This may be because Viwandani, being in the industrial area and alluring labourers to the industries is likely to accept more educated people (other than the mother) for example the father and other household members, who may touch on baby feeding practices. Mothers who delivered at home were more probable to innovate complementary foods earlier than those who delivered in a health facility. Mothers who evangelize in a health facility in nigh cases receive breastfeeding counselling, especially with the revitalisation of the Infant Friendly Hospital Initiative (BFHI) from 2007 aimed at promoting optimal breastfeeding practices. The BFHI has been found to be constructive in several settings in the developing world [47]. BFHI, is being revitalized in Kenya in the National Strategy on Baby and Immature Child feeding [12], and information technology may be playing a role in encouraging mothers to exclusive breastfeeding their infants in the first 6 months of life. Since the BFHI initiative was introduced, there has been potential improvement in the proportion of children exclusively breastfed from thirteen% in 2003 to 32% in 2008 [x]. The positive association between pregnancy desirability and complementary feeding has barely been previously studied. In our study, infants who were unwanted at conception but were wanted later were less likely to exist introduced to complementary foods early. The association between pregnancy desirability and breastfeeding and complementary feeding practices needs further investigation.
Urban slum settings present unique challenges with regards to breastfeeding and infant and young kid feeding practices due to their physical and socio-economic characteristics. In these informal settings, bones authorities services including health care services are limited and this, coupled with financial constraints, leads to a substantial proportion of women in these slums giving birth at home or at breezy private health facilities [48, 49]. This ways that nearly of these slum women are systematically excluded from regime initiatives such as those aimed at promoting optimal breastfeeding and babe feeding practices, based at health facilities such as the BFHI mentioned above, which involves counselling of mothers on infant and immature child feeding effectually the time of delivery. Another unique characteristic of slum settings is limited livelihood opportunities [15] hence food insecurity. As indicated in this report and in other slums such as in India [31], ane key reason for initiating complementary foods likewise early on is due to the mother having inadequate breast milk. While the of import part of hormones and the psychosocial status of the female parent in lactation is well established, though express bear witness exists, book of milk produced may also be related to maternal nourishment. A review of breastmilk volumes and composition amidst poorly nourished communities indicated that milk volumes were everyman in communities with poor levels of nutrition and poor living conditions [fifty].
Potential interventions to accost the unique challenges in the slum settings should address both admission problems and the socio-economic limitations. A potential intervention to annul the systematic exclusion from basic government services may include, home-based counselling of mothers on infant and young child feeding by customs based health workers and/or supporting the (informal) private service providers for instance through grooming programs to offer services according to established regime guidelines such as those on breastfeeding. The effectiveness of such interventions in health care delivery, including promotion of optimal infant feeding practices in resource-constrained settings has been indicated [51]. To raise adequacy of milk produced by the mothers, potential interventions may be to heighten maternal nourishment through ensuring nutrient security. This may be through advisable income generating activities to raise livelihoods. Nutrient supplementation has also been institute to heighten breastmilk volume [50]. Additionally, interventions that empower the new mother by demonstrating correct breastfeeding techniques, ways of stimulating breast milk production, and counselling on proper diet may ameliorate breastfeeding practices [52].
Limitations in this study chronicle to missing values in some of the variables particularly the socio-economic status variables. Advisable measures were taken in the analysis to minimize bias as indicated above. It would have been of import to follow-upwardly the children for a longer period to constitute complete elapsing of breastfeeding in line with the WHO recommendation that breastfeeding should continue for ii years or beyond. This was however not done and children were merely followed upward till they were slightly more than 1 year old. Despite these limitations, this study has primal strengths that are worth mentioning. The study provides of import information on babe breastfeeding and feeding practices in breezy settings in sub-Saharan Africa, for which there is a dearth. A key strength of this study lies in its longitudinal nature, minimising call up bias that may be associated with cross-sectional studies. The report involved rigorous follow-upwardly hence information for most of the children was updated by the stop of the follow-up period, reducing bias due to loss to follow-up. The study involved a demography of all children born to mothers in two defined geographical areas; hence there was minimal bias due to sampling error.
Conclusion
This study presents important findings on breastfeeding and babe feeding practices and determinants of sub-optimal practices in informal settings in sub-Saharan Africa. This is timely and critical as such testify is currently rare. The study finds that despite universal breastfeeding in this population, WHO breastfeeding and baby feeding recommendations are rarely adhered to. It is important therefore to develop interventions targeting women, wellness intendance workers and policy makers aimed at bridging the gap between current breastfeeding and infant feeding practices in the informal settings and WHO recommendations. It is evident from this report that breastfeeding and baby feeding patterns are associated with kid, maternal and household level factors and it is crucial to understand and reduce the inequalities. Interventions and farther research should address inequalities including gender, ethnicity, access to and utilization of wellness intendance facilities, socio-economical condition and family planning. This study only looked at early introduction of complementary food; further investigation on late introduction of the same is needed.
Abbreviations
- APHRC :
-
African Population and Health Enquiry Center
- BFHI :
-
Baby Friendly Hospital Initiative
- HIV :
-
Human Immuno-deficiency Virus
- NUHDSS :
-
Nairobi Urban Health and Demographic Surveillance Arrangement
- HR :
-
Hazard Ratio
- TBA :
-
Traditional Birth Attendant
- UNICEF :
-
United Nations Children's Educational activity Fund
- United states of america:
-
United States
- WHO :
-
World Health Organisation.
References
-
Victora CG, Adair 50, Fall C, Hallal PC, Martorell R, Richter L, Sachdev HS, Maternal and Child Undernutrition Study G: Maternal and kid undernutrition: consequences for developed health and human capital. Lancet. 2008, 371: 340-357. x.1016/S0140-6736(07)61692-4.
-
Grantham-McGregor South, Cheung YB, Cueto S, Glewwe P, Richter 50, Strupp B: Developmental potential in the first 5 years for children in developing countries. Lancet. 2007, 369 (9555): lx-70. ten.1016/S0140-6736(07)60032-4.
-
Oddy WH, Kendall GE, Blair E, De Klerk NH, Stanley FJ, Landau LI, Silburn S, Zubrick South: Breast feeding and cognitive development in childhood: a prospective nativity cohort study. Paediatr Perinat Epidemiol. 2003, 17 (1): 81-90. 10.1046/j.1365-3016.2003.00464.ten.
-
Kramer MS, Kakuma R: The optimal duration of exclusive breastfeeding: a systematic review. Adv Exp Med Biol. 2004, 554: 63-77.
-
Gareth J, Richard WS, Robert EB, Zulfiqar AB, Saul SM: How many child deaths can we forbid this year?. Lancet. 2003, 362 (9377): 65-71. ten.1016/S0140-6736(03)13811-i.
-
WHO: The optimal duration of exclusive breastfeeding. Study of an Skillful Consultation. 2002, Geneva: WHO, Accessed December 2010, [http://whqlibdoc.who.int/hq/2001/WHO_NHD_01.09.pdf]
-
Arifeen Due south, Black RE, Antelman G, Baqui A, Caulfield L, Becker S: Exclusive breastfeeding reduces astute respiratory infection and diarrhea deaths amidst infants in Dhaka slums. Pediatrics. 2001, 108 (4): E67-x.1542/peds.108.4.e67.
-
WHO: Global strategy for infant and young child feeding. 2003, Geneva: WHO, Accessed December 2010, [http://world wide web.paho.org/english/ad/fch/ca/GSIYCF_infantfeeding_eng.pdf]
-
Lauer J, Betran A, Victora C, de Onis M, Barros A: Breastfeeding patterns and exposure to suboptimal breastfeeding amongst children in developing countries: review and assay of nationally representative surveys. BMC Medicine. 2004, two (1): 26-x.1186/1741-7015-2-26.
-
Kenya National Agency of Statistics (KNBS), ICF Macro: Kenya Demographic and Health Survey 2008-09. 2009, Calverton, Maryland: KNBS and ICF Macro, Accessed Jan 2011, [http://www.measuredhs.com/pubs/pdf/FR229/FR229.pdf]
-
Central Bureau of Statistics (CBS) Republic of kenya, Ministry of Health (MoH), Kenya, ORC Macro: Kenya Demographic and Health Survey 2003: Key Findings. 2004, Calverton, Maryland, The states: CBS, MOH and ORC Macro, Accessed January 2011, [http://www.measuredhs.com/pubs/pdf/SR104/SR104KE03.pdf]
-
Ministry of Public Health and Sanitation: National Strategy on Infant and Young Child Feeding Strategy 2007-2010. 2007, Nairobi: Ministry of Public Health and Sanitation, Kenya, Accessed January 2011, [http://www.hennet.or.ke]
-
UNHABITAT: Slums of the World. The Confront of Urban Poverty in the New Millennium? Global Urban Observatory. 2003, Nairobi: UNHABITAT, Accessed January 2011, [http://www.unhabitat.org/pmss/listItemDetails.aspx?publicationID=1124]
-
African Population and Health Enquiry Center: Population and Health Dynamics in Nairobi Informal Settlements. 2002, Nairobi: APHRC, Accessed January 2011, [http://www.aphrc.org/insidepage/page.php?app=publications1]
-
African Population and Health Research Center: Health and Livelihood Needs Of Residents of Informal Settlements on Nairobi City. Occasional Study Report one. 2002, Nairobi: APHRC, Accessed January 2011, [http://www.aphrc.org/insidepage/page.php?app=publications1]
-
Kimani-Murage EW, Ngindu AM: Quality of water the slum dwellers use: the case of a Kenyan slum. J Urban Wellness. 2007, 84 (6): 829-838. 10.1007/s11524-007-9199-10.
-
Mutua MK, Kimani-Murage Due east, Ettarh RR: Childhood vaccination in informal urban settlements in Nairobi, Kenya: Who gets vaccinated?. BMC Public Health. 11 (1): 6-
-
Fotso JC: Urban-rural differentials in child malnutrition: trends and socioeconomic correlates in sub-Saharan Africa. Health Place. 2007, 13 (1): 205-223. ten.1016/j.healthplace.2006.01.004.
-
Patel A, Badhoniya N, Khadse S, Senarath U, Agho KE, Dibley MJ: Infant and young child feeding indicators and determinants of poor feeding practices in India: secondary data analysis of National Family Health Survey 2005-06. Food Nutr Bull. 31 (2): 314-333.
-
Roig AO, Martinez MR, Garcia JC, Hoyos SP, Navidad GL, Alvarez JC, Pujalte Mdel M, De Leon Gonzalez RG: Factors associated to breastfeeding abeyance before 6 months. Rev Lat Am Enfermagem. xviii (3): 373-380.
-
Kristiansen AL, Lande B, Overby NC, Andersen LF: Factors associated with exclusive breast-feeding and chest-feeding in Norway. Public Health Nutr. 1-x.
-
Thulier D, Mercer J: Variables associated with breastfeeding duration. J Obstet Gynecol Neonatal Nurs. 2009, 38 (3): 259-268. 10.1111/j.1552-6909.2009.01021.x.
-
Scott JA, Binns CW: Factors associated with the initiation and duration of breastfeeding: a review of the literature. Breastfeed Rev. 1999, vii (1): v-xvi.
-
Pascale KNA, Laure NJ, Enyong OJ: Factors Associated with Breast feeding equally Well as the Nutritional Status of Infants (0-12) Months: An Epidemiological Study in Yaounde, Republic of cameroon. Pakistan J Nutr. 2007, 6 (iii): 259-263.
-
Akter S, Rahman MM: The determinants of early cessation of breastfeeding in Bangladesh. Earth Health Popul. 11 (4): 5-12.
-
Engebretsen IM, Wamani H, Karamagi C, Semiyaga Due north, Tumwine J, Tylleskar T: Depression adherence to exclusive breastfeeding in Eastern Uganda: a community-based cross-exclusive written report comparing dietary recall since birth with 24-hour remember. BMC Pediatr. 2007, 7: 10-x.1186/1471-2431-7-10.
-
Mihrshahi S, Kabir I, Roy SK, Agho KE, Senarath U, Dibley MJ: Determinants of baby and immature kid feeding practices in Bangladesh: secondary data analysis of Demographic and Health Survey 2004. Food Nutr Balderdash. 31 (two): 295-313.
-
Davies-Adetugbo AA: Sociocultural factors and the promotion of exclusive breastfeeding in rural Yoruba communities of Osun State, Nigeria. Soc Sci Med. 1997, 45 (ane): 113-125. x.1016/S0277-9536(96)00320-6.
-
Onyango AW, Esrey SA, Kramer MS: Connected breastfeeding and child growth in the second twelvemonth of life: a prospective cohort study in western Republic of kenya. Lancet. 1999, 354 (9195): 2041-2045. ten.1016/S0140-6736(99)02168-half dozen.
-
Madise NJ, Mpoma M: Child malnutrition and feeding practices in Republic of malaŵi. Food Nutr Bull. 1997, 18 (2): 190-201.
-
Roy S, Dasgupta A, Pal B: Feeding practices of children in an urban slum of Kolkata. Indian J Community Med. 2009, 34 (4): 362-363. 10.4103/0970-0218.58402.
-
Tiwari R, Mahajan PC, Lahariya C: The determinants of exclusive breast feeding in urban slums: a customs based study. J Trop Pediatr. 2009, 55 (1): 49-54.
-
Madise NJ, Matthews Z, Margetts B: Heterogeneity of kid nutritional status between households: A comparison of half-dozen sub-Saharan African countries. Population Stud. 1999, 53 (3): 331-343.
-
Dewey KG: Nutrition, growth, and complementary feeding of the breastfed infant. Pediatr Clin North Am. 2001, 48 (1): 87-104. 10.1016/S0031-3955(05)70287-X.
-
Arifeen S, Blackness R, Antelman G, Baqui A, Caulfield L, Becker S: Sectional breastfeeding reduces astute respiratory infection and diarrhea deaths amidst infants in Dhaka slums. Pediatrics. 2001, 108: E67-x.1542/peds.108.four.e67.
-
Chikusa Madise NJ: Effects of breastfeeding on infant and kid morbidity and malnourishment [in Botswana] using the multinomial logistic model. Biometry for Development, Proceedings of the First Scientific Coming together of the Biometric Gild, Nairobi, Kenya 2-six April 1990. Edited past: Patel MS, Nokoe S. 1991, Nairobi: ICIPE Science Press, 187-193.
-
Haider R, Rasheed S, Sanghvi TG, Hassan N, Pachon H, Islam S, Jalal CS: Breastfeeding in infancy: identifying the programme-relevant bug in Bangladesh. Int Breastfeed J. 5: 21-
-
Martines JC, Ashworth A, Kirkwood B: Chest-feeding amidst the urban poor in southern Brazil: reasons for termination in the first six months of life. Bull Earth Health Organ. 1989, 67 (2): 151-161.
-
Giugliani ER: [Breast-feeding: how and why to promote information technology]. J Pediatr (Rio J). 1994, 70 (3): 138-151.
-
Ministry of Wellness, Government of Kenya: National Guidelines on Diet and HIV/AIDS. 2006, Nairobi, Accessed May 2011, [http://world wide web.fantaproject.org/downloads/pdfs/Kenya_Nutrition_Guidelines_2006.pdf]
-
Ziraba AK, Madise NJ, Matilu 1000, Zulu E, Kebaso J, Khamadi S, Okoth V, Ezeh AC: The effect of participant nonresponse on HIV prevalence estimates in a population-based survey in two informal settlements in Nairobi city. Popul Health Metr. 2010, 8: 22-10.1186/1478-7954-viii-22.
-
Kennedy KI, Kotelchuck G: Policy considerations for the introduction and promotion of the lactational amenorrhea method: advantages and disadvantages of LAM. J Hum Lact. 1998, 14 (3): 191-203. 10.1177/089033449801400303.
-
Hediger ML, Overpeck Doctor, Ruan WJ, Troendle JF: Early baby feeding and growth status of US-born infants and children aged 4-71 mo: analyses from the tertiary National Wellness and Diet Examination Survey, 1988-1994. Am J Clin Nutr. 2000, 72 (i): 159-167.
-
Lande B, Andersen LF, Baerug A, Trygg KU, Lund-Larsen K, Veierod MB, Bjorneboe GE: Infant feeding practices and associated factors in the outset half dozen months of life: the Norwegian infant nutrition survey. Acta Paediatr. 2003, 92 (2): 152-161.
-
Wijndaele K, Lakshman R, Landsbaugh JR, Ong KK, Ogilvie D: Determinants of early on weaning and utilise of unmodified moo-cow'southward milk in infants: a systematic review. J Am Diet Assoc. 2009, 109 (12): 2017-2028. x.1016/j.jada.2009.09.003.
-
Ku CM, Chow SK: Factors influencing the practice of sectional breastfeeding amid Hong Kong Chinese women: a questionnaire survey. J Clin Nurs. 19 (17-eighteen): 2434-2445.
-
Braun ML, Giugliani ER, Soares ME, Giugliani C, de Oliveira AP, Danelon CM: Evaluation of the touch of the baby-friendly hospital initiative on rates of breastfeeding. Am J Public Health. 2003, 93 (eight): 1277-1279. 10.2105/AJPH.93.viii.1277.
-
Fotso J-C, Ezeh A, Madise N, Ziraba A, Ogollah R: What does access to maternal care mean among the urban poor? Factors associated with use of appropriate maternal health services in the slum settlements of Nairobi, Kenya. Matern Child Health J. 2009, 13 (1): 130-137. 10.1007/s10995-008-0326-4.
-
Essendi H, Mills S, Fotso JC: Barriers to formal emergency obstetric care services' utilization. J Urban Health.
-
Jelliffe DB, Jelliffe EF: The volume and composition of human milk in poorly nourished communities. A review. Am J Clin Nutr. 1978, 31 (three): 492-515.
-
Haider R, Ashworth A, Kabir I, Huttly S: Upshot of community-based peer counsellors on exclusive breastfeeding practices in Dhaka, Bangladesh: a randomised controlled trial. Lancet. 2000, 356: 1643-1647. 10.1016/S0140-6736(00)03159-7.
-
Mellin PS, Poplawski DT, Gole A, Mass SB: Impact of a formal breastfeeding education program. MCN Am J Matern Child Nurs.
Pre-publication history
-
The pre-publication history for this newspaper can be accessed here:http://www.biomedcentral.com/1471-2458/11/396/prepub
Acknowledgements
This study was funded by the Wellcome Trust (Grant No. 078530/Z/05/Z). We also acknowledge funding for the NUHDSS from the Rockefeller Foundation and core back up for APHRC from the Rockefeller Foundation, the William and the Flora Hewlett Foundation. We would similar to thank Dr. Alex Ezeh, Dr. Eliya Zulu, Prof. John Cleland, Prof Jane Falkingham and Prof Philippe Bocquier for their contribution in the design of the study from which data for this article was derived. We thank Dr. George Mgomella, Ms Hilda Essendi, Ms Teresa Saliku and Mr. Peter Muriuki for project coordination. We are also grateful to the data drove team and the data processing and management squad at APHRC. We are highly indebted to the study participants.
Author information
Affiliations
Corresponding author
Boosted data
Competing interests
The authors declare that they accept no competing interests.
Authors' contributions
EWK-Chiliad:Blueprint of the report, projection management, data analysis, writing of the manuscript and approval for submission; NJM: Principal Investigator of the project, design of the study, analytic guidance, reviewing of the manuscript and approval for submission; J-CF: Design of the study, overall project co-ordination, reviewing of the manuscript and approval for submission; CK: Design of the study, projection management, review of the manuscript and approval for submission; MK: Information management and analysis, review of the manuscript and approval for submission; TG: Writing of the manuscript and approval for submission; NY: Writing of the manuscript and approval for submission. All authors read and approved the final manuscript.
Authors' original submitted files for images
Rights and permissions
This commodity is published nether license to BioMed Cardinal Ltd. This is an Open Access article distributed under the terms of the Creative Commons Attribution License (http://creativecommons.org/licenses/by/2.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Reprints and Permissions
Nearly this commodity
Cite this commodity
Kimani-Murage, Eastward.W., Madise, North.J., Fotso, JC. et al. Patterns and determinants of breastfeeding and complementary feeding practices in urban informal settlements, Nairobi Kenya. BMC Public Health eleven, 396 (2011). https://doi.org/10.1186/1471-2458-11-396
-
Received:
-
Accepted:
-
Published:
-
DOI : https://doi.org/ten.1186/1471-2458-xi-396
Keywords
- Breast Milk
- Exclusive Breastfeed
- Feeding Practice
- Urban Slum
- Early Introduction
williamsthadmilly.blogspot.com
Source: https://bmcpublichealth.biomedcentral.com/articles/10.1186/1471-2458-11-396
0 Response to "Kenya and Satoru Meet Again but Meet a Child That Breastfeeding From Satoru Fanfic"
Post a Comment